
Dear colleagues,
Welcome to our spring and summer news 2023! Temperatures have risen in Europe and holiday season just started. We hope you are doing fine at your place!
We are pleased to offer you a choice of articles on neuromuscular ultrasound that were published in the first half of 2023.
This time it´s review time! This especially concerns neuromuscular ultrasound in children. So if this is your topic, you should find some information here – from optic nerve ultrasound, to nerve trauma and also reference values according to age. The other papers offer a broad variation on different topics you should have a look at, covering some new approaches to entrapment neuropathy with longitudinal imaging of the ulnar nerve at the elbow or a scanning protocol for CIDP including only the median and ulnar nerve.
We hope you’ll enjoy your read.
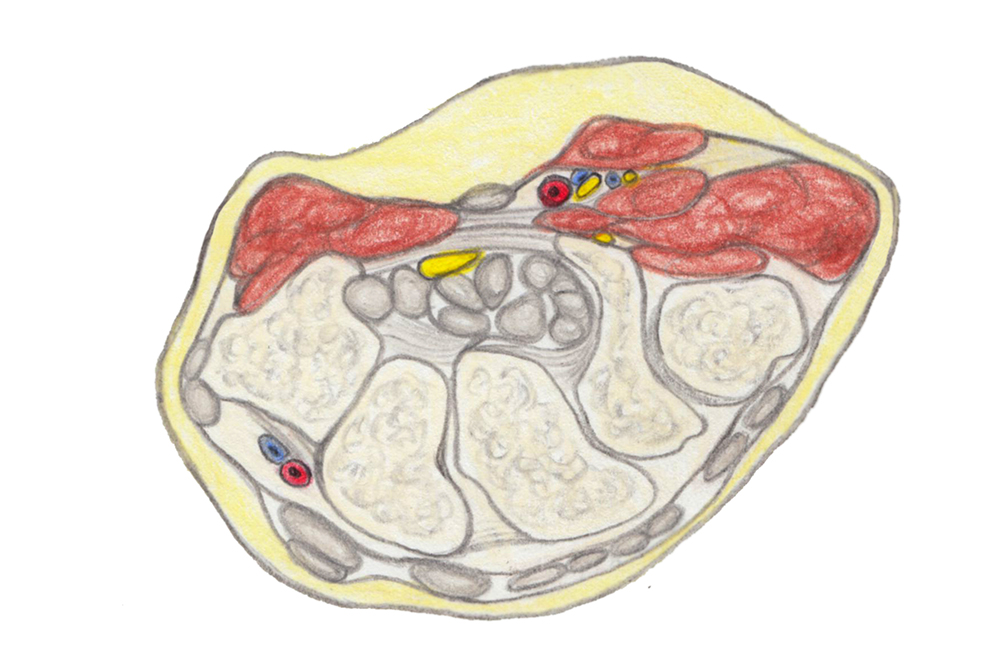
© Gerlinde Maria Gruber,2019
CARPAL TUNNEL SYNDROME & OTHER ENTRAPMENT NEUROPATHIES
Aloi et al. Ultrasound cross-sectional area of the median nerve is not a predictor of patient reported outcomes after carpal tunnel release. Hand (N.Y.) 2023; 18 (1_suppl): 114s-8s
The study examines whether pre-operative CSA of the median nerve is a predictor of outcome after carpal tunnel release. For this purpose, CSAs and BCTQ scores of patients with numbness and tingling of the upper extremity were collected at a center for six years. Patients were divided into a US-positive and US-negative group with a cut-off of 10 mm2. There was no difference between the two groups and CSA is therefore not a predictor for outcome after CT-release.
Sertbas et al. The role of ultrasound in determining the presence and severity of carpal tunnel syndrome in diabetic patients. J Investig Med 2023 May 6th, online ahead of print.
The median nerves of the wrist were measured in 128 randomly selected patients with DM II, of whom 28% had CTS. The median CSA was higher in patients with CSA, but did not correspond to the severity of clinical grading in minimal, mild and moderate CTS groups. The authors concluded that US can be used as a diagnostic tool in clinically severe cases, but not in the other ones.
*Pardal-Fernández et al. Ulnar nerve thickness at the elbow on longitudinal ultrasound view in control subjects. Neurol Res Pract 2023; 5 (1):4
Interesting approach to ulnar neuropathy at the elbow. Nowadays the cross-sectional area is the most frequently used parameter for diagnosing nerve pathology on ultrasound. The authors examined changes of diameter in longitudinal view of the ulnar nerve around the elbow in healthy subjects. They were around 2 mm, with slight differences between the proximal and distal ulnar groove. The authors suggest further studies to determine the diagnostic value of this simple and fast method. Similar approaches for diagnosing carpal tunnel syndrome did not prove successful.

© Pexels.com
NERVE TRAUMA
Fu et al. High-resolution ultrasound imaging of axillary nerve and relevant injury. J Ultrasound Med 2023; doi: 10.1002/jum.16233 online ahead of print
The authors describe the common technique of visualizing the axillary nerve in the quadrilateral space 15 cases of patients with axillary nerve injury, in which 12 had a diffuse swelling and three a discontinuity and ultrasound helped in establishing the diagnosis.
Samet. Ultrasound in peripheral nerve injury. Pediatr Radiol 2023, doi: 10.1007/s00247-023-05631-8. online ahead of print
This review summarizes changes in peripheral nerve injury with special regard to differentiating high and low grade injury – which is important considering different therapeutic approaches.
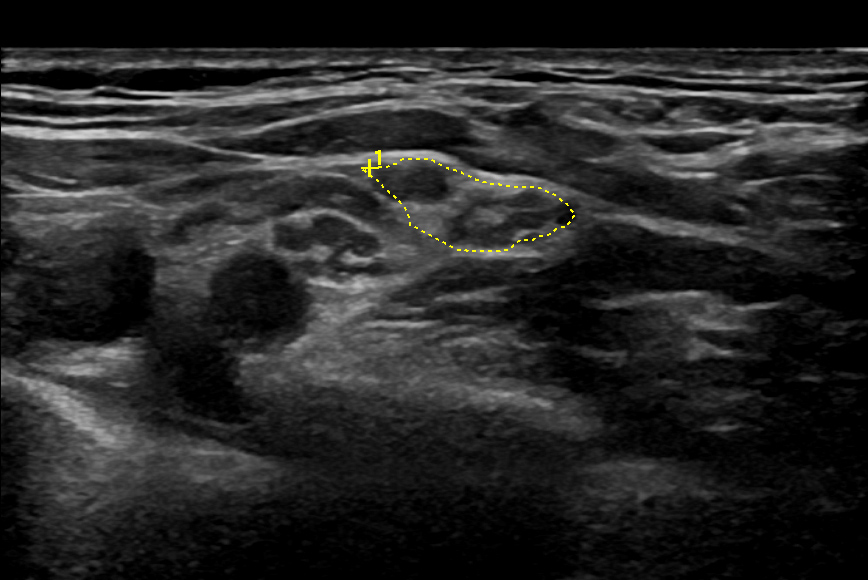
POLYNEUROPATHY
*Klawitter et al. Neuromuscular ultrasound in intensive care unit-acquired weakness: current state and future directions. Medicina 2023; 59: 884
This narrative review sums up the current evidence especially on muscle ultrasound techniques for assessment of critical illness myopathy and/or polyneuropathy. Nerve ultrasound surely plays a minor role in this topic and to date we only know that CSA is not useful in distinguishing patients with and without ICU-acquired weakness.
For IC-myopathy different parameters have been assessed, including muscle layer thickness and muscle CSA for quantification of muscle mass and quantitative rating either by the examiner with the Heckmatt scale or automated analysis – which both seem promising and warrant further investigation.
Yun et al. Focused neuromuscular ultrasound approach for the diagnosis of chronic inflammatory demyelinating polyneuropathy. J Clin Neurophysiol 023; 40 (4): 378-81
The authors of this study prospectively examined the ulnar and median nerves of 25 patients with diagnosed CIDP. They found enlargement in at least one segment in all subjects and concluded that this simple approach may help establish the diagnosis of CIDP.
It would of course be great if these nerves whose scanning is so simple would help with the diagnosis, but so far the protocols that were examined in larger studies did not get along without scanning of at least one cervical root.
NERVE TUMORS
Lefebvre and Le Corroller. Ultrasound and MR imaging of peripheral nerve tumors: the state of the art. Skeletal Radiology 2023; 52: 405-19
Highly compressed information on nerve sheath tumors, not going too much into detail (as this would surely be too much for a paper), but providing the most important points on PNST and an elaborated list on other tumor entities and also pseudotumors.

© Adobe Stock
REFERENCE VALUES
*Abdelnaby et al. Sonographic reference. Values of nerve size in children: a systematic review and meta-analysis. Muscle Nerve 2023; 67 (3): 217-25
Free review article presenting an overview of 16 studies in healthy children, summarizing results in growth charts for major limb nerves. If you scan children regularly, this might be of interest to you.
TECHNIQUE
*Jerban et al. Quantitative ultrasound techniques used for peripheral nerve assessment. Diagnostics 2023; 13 (5): 956
This article provides an overview of approaches for an objective evaluation of changes in echogenicity observed in neuropathy. B-mode echogenicity indexes, elastography and raw backscattered ultrasound radiofrequency signals are presented with background of technique and currently available literature with regard to peripheral nerve disorders. Furthermore, current pitfalls are highlighted.
OPTIC NERVE ULTRASOUND
*Abbinante et al. Optic nerve ultrasound evaluation in children: a review. Diagnostics 2023; 13 (3): 535
Good overview of the current literature on optic nerve ultrasound in children and they give cut-off values if available. While in adults optic nerve ultrasound has mostly been used to monitor for elevated intracranial pressure related to head trauma, studies in children offer data in a wide variety of pathological conditions like cardiac surgery with cardiopulmonary bypass, cranial synostosis, ventriculo-peritoneal shunt failure, diabetic ketoacidosis or malaria caused by plasmodium falciparum.

© Pexels.com
SMALL NERVES
*Heiling et al. Evaluating diagnostic ultrasound of the vagus nerve as a surrogate marker for autonomic neuropathy in diabetic patients. Medicina 2023; 59: 525
The CSA of the vagus nerve was measured in 111 patients with type 2 diabetes and compared to 104 healthy adults and 41 patients with CIDP. In the diabetes group, sympathetic skin response served as a marker for autonomic dysfunction (absent in 23.4% of patients) and carotid intima-media thickness as a marker for artherosclerosis. There was no correlation between vagus nerve CSA, CIMT or SSR in diabetic patients. The right vagus was statistically significantly larger in patients with DMII and CIDP than in healthy controls, but with only a small difference. Vagus nerve CSA does not seem to indicate autonomic dysfunction or cardiovascular risk in patients with DM II.
THE INTERESTING CASE
Wada et al. Utility of nerve ultrasound in the management of primary neurolymphomatosis: case report and review of the literature. Clin Neurophysiol Pract 2023; 8: 92-6
Just a reminder that ultrasound can be useful in neurolymphomatosis.
Ok… now that was a lot to go through. We hope you liked our news and can use some of the information for yourself. If you have any comments or if we have missed your most important paper, just leave us a comment!
Stay safe, see you soon.
Your Sonocampus Team
*This is a free article

Great. Thank you. This is very helpful. I wasn't aware of half of these publications!
How do you select your articles? I am asking, because there are a few missing, which are quite relevant to our discipline.
Dear Dr. Pelosi!
Thank you for your kind comment. We feel very honored to hear from you and know you got our newsletter. We do a review of articles published in a certain time frame in Pubmed and MEDLINE databases using keywords like "neuromuscular ultrasound", "nerve ultrasound", then adding combinations with the major limb nerves/plexus and disorders to see what is new. Of course we are a little bit limited with number of articles we can talk about and this is why we ask our readers to let us know if we missed anything that is important from their side. If you have any suggestions, we are happy to hear them!
Best regards
Doris Lieba-Samal