
Dear readers,
Welcome to our Spring Newsletter 2021! Let´s use the time to get a little distraction from the pandemic that is still not over, and allow us to shift your attention to a different topic for some moments: neuromuscular ultrasound.
If you would like to summarize the hottest news in latest publications in the field of NMUS, the title should be: “A look into a bright future”. Currently many groups are working on pushing borders in diagnosing and treating with ultrasound beyond use of traditional cross-sectional area. Experiments are going on with elastography, speckle tracking, contrast-enhanced ultrasound and artificial intelligence. Also vascularity, which was already a topic in early days of compression syndromes, but then not turned out to be the distinguishing point, is among candidates for diagnosis again.
Furthermore we hear about ultrasound and its usefulness in leprotic neuropathy. CIDP and differential diagnosis are on the list, as well as news about small nerves – have you ever heard about Berrettinis anastomosis? And finally: interesting news about treatment of carpal tunnel syndrome with hydrodissection.
As always please note that we can just pick out a few papers. If we missed your most important paper from the past months – just let us know.

IF YOU START OUT…
Ultrasound scanning in the diagnosis of peripheral neuropathies
Telleman et al. Pract Neurol 2021, epub ahead of print Feb 4
The most recent review providing an overview on the possibilities of neuromuscular ultrasound in mono- and polyneuropathy.

WHAT YOU SEE BESIDES THE NERVE…
Managing uncommon and unexpected findings during neuromuscular ultrasound
Walker F, Cartwright M, Hunt C. Muscle Nerve 2020 Dec 15, online ahead of print.
Depending on your background, you might be interested in that one. If you are a radiologist or sonographer, you are surely familiar with common pathologies or anatomic variants of tissues besides nerves and muscles. If you come from a different field of work, which e.g. focuses on clinical examination, you might not be that confident about lymph nodes and lipomas, however. Then this article helps you out.
Musculoskeletal ultrasound for traumatic and torsional alterations
Strakowski J, Chiou-Tan F. Muscle Nerve 2020; 62 (6)654
This review provides an overview on everything that can appear in connection with a trauma – muscle as well as nerve injury.

A LOOK INTO THE FUTURE
*Current and future applications of ultrasound imaging in peripheral nerve disorders.
Carroll A, Simon N. WJR 2020; 12(6):101
Emerging technologies in neuromuscular ultrasound
Hobson-Webb L. Muscle Nerve 2020; 61(6)
In this review we hear about elastography, photoacoustic imaging and artificial intelligence and how these techniques might help us with diagnosing peripheral nerve disorders in the future.
*Recent advances in ultrasound diagnosis of carpal tunnel syndrome
Yoshii Y, Zhao C, Amadio A. Diagnostics 2020
If you think everything has been said about CTS and US then you are wrong. Measuring the cross-sectional area for diagnosis might be old-fashioned in some years. This paper presents potential new techniques for diagnosing the most frequent compression syndrome. If you want to get an idea of techniques on the way, check this one out.
HYDRODISSECTION
*Ultrasound-guided nerve hydrodissection for pain management: rationale, methods, current literature and theoretical mechanisms
Lam K, Hung C, Chiang Y, Onishi K, Su D, Clark T, Reeves K. J Pain Res 2020 Aug; 13:1957
Good if you are thinking about starting out with hydrodissection and would like to get an overview on current literature. Provides some nice videos on the procedure itself.
Ultrasound imaging and guidance in peripheral nerve entrapment: hydrodissection highlighted
Chang K, Wu W, Özcakar L
*Prognostic factors in carpal tunnel syndrome treated with 5% dextrose perineural injection: a retrospective study
Ho et al. Int J Med Sci 2021; 18(9):1960-5
A retrospective study of 52 patients looking for factors that help you to define which patients will profit most from hydrodissection in CTS. They dichotomized in good versus bad outcome with symptom relief >/<50% reduction in pain, measured with VAS 0-10. In stepwise regression analysis only sensory nerve conduction velocity remained significant, with those with lesser reduction (33.6+/- 0,8) had a better outcome. This may indicate that only the milder forms of CTS will profit more.
CORTICOSTEROID INJECTIONS IN CARPAL TUNNEL SYNDROME
Ultrasound-guided perineural vs. peritendinous corticosteroid injections in carpal tunnel syndrome: a randomized controlled trial
Mezian et al. Eur J Phys Rehabil Med 2021; epub ahead of print
The authors checked if the injection site – next to the median nerve (n=23) vs. among flexor tendons (n=23) – has a substantial impact on outcome. Again, the VAS was the primary outcome measure. After 2,6 and 12 weeks, no difference could be detected between the groups. The authors concluded that both injection sites are equally effective and safe.
BABYLON
*AANEM- IFCN Glossary of terms in neuromuscular electrodiagnostic medicine and ultrasound
Dengler R et al. Muscle Nerve 2020; 62 (1): 10
Providing us with a common language for describing our results.
LEPROSY
*High-resolution ultrasound in the assessment of peripheral nerves in leprosy: a comparative cross-sectional study
Sreejith K. et al. Indian J Dermatol Venereol Leprol 2021; 87(29), 199-206
Nerve thickening in leprosy is important for classification and treatment of the disease. The authors compared detection rate of nerve swelling in clinical vs. ultrasound. Overall, HRUS detected 41% of 300 nerves enlarged compared to 20% diagnosed by clinical examination. There was a big difference especially in nerves without impairment of function. The authors concluded that HRUS may improve the sensitivity of the diagnostic criterion of peripheral nerve enlargement.
Akita J et al. Comparison between nerve conduction study and high-resolution ultrasonography with color doppler in type 1 and type 2 leprosy patients.
Clin Neurophysiol Pract 2021; 6, 97-102
The authors evaluated 257 nerves in 35 leprosy patients with signs or symptoms suggestive of inflammatory activity by means of NCS and ultrasound. Subacute segmental demyelination and presence of blood flow were considered to signify IA.
Inflammatory activity was detected in 68% of patients with NCS vs. 74% with US. Combining the methods resulted in diagnostic rate of 91%.
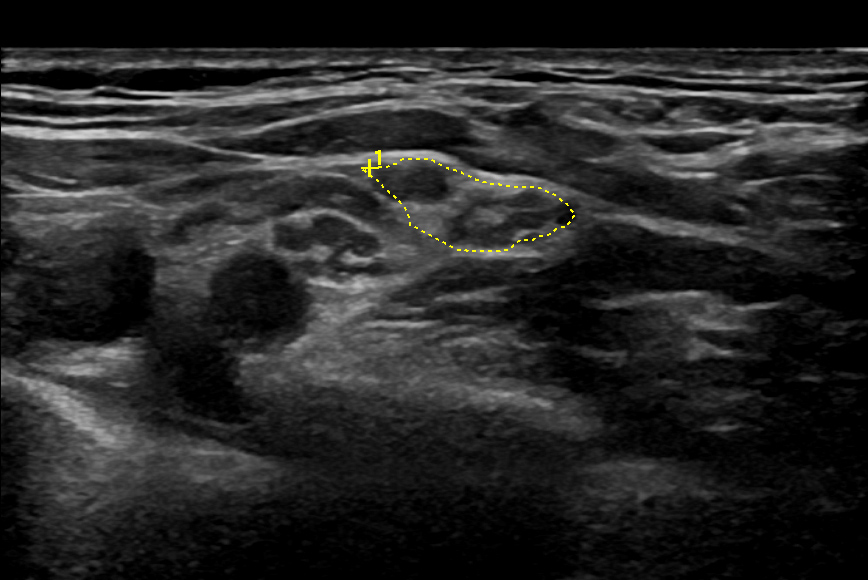
CHRONIC INFLAMMATORY DEMYELINATING POLYNEUROPATHY and DIFFERENTIALS
Nerve ultrasound comparison between transthyretin familial amyloid polyneuropathy and chronic inflammatory demyelinating polyneuropathy
Du et al. Front Neurol 2021; 12; 632096
TTR-FAP and CIDP are important differential diagnoses, because they can be treated effectively, but need different treatments. Both can manifest as rapid onsetting polyneuropathy and might show demyelinating features in NCS, therefore leading to misdiagnosis.
Patients with TTR-FAP (n=18), CIDP (n=13) and healthy controls (n=14) were scanned along upper and lower extremity nerves – measuring CSA at multiple sites. Generally, there was a milder enlargement in TTR-FAP than in CIDP. However, the difference was not enough to create a credible index to differentiate between the two disorders. Variability of the median nerve along its course was significantly higher in CIDP, but also only with a sensitivity of 69% and a specificity of 83%. The authors conclude that the variability may a useful tool for differentiating these neuropathies.
Conclusion: not ready for use in your ultrasound-lab. Further studies needed.
Changes of clinical, neurophysiological and nerve ultrasound characteristics in CIDP over time: a 3-year follow up.
Fioda et al. J Neurol 2021, epub ahead of print
23 patients with CIDP were followed for 3 years. The interesting part: during FU, the CSA increased in half of the nerve segments and correlated with INCAT increase and NCV and cMAP reduction.
High-resolution nerve ultrasound abnormalities in POEMS syndrome – a comparative study
Dörner et al. Diagnostics 2021; 11 (2): 264
POEMS syndrome (polyneuropathy, organomegaly, endocrinopathy, M-protein, skin changes) is rare, but might be mixed up with CIPD. A case series of three patients with POEMS syndrome is compared to CIDP patients and controls. Both groups of patients showed enlargement of various nerves, which did not turn out as being a distinguishing feature between the two disorders. However, the POEMS patients were found to have a specific pattern of alteration – hypoechoic fascicles with increased hyperechoic intraneural connective tissue. Future studies will be needed.

SMALL NERVES
High-resolution songraphic study of the communicating branch of Berrettini: an anatomic feasibility study
Dukan et al. J Hand Surg Eur 2021, epub ahead of print Mar 12.
The Berrettini branch is an interesting thing – explaining why a patient with an ulnar neuropathy can have involvement of the third finger JNow it has also documented with ultrasound. This could avoid complications in carpal tunnel surgery.
If you got interested but don´t have access, have a look at this one:
Comprehensive summary of anastomoses between the median and ulnar nerves in the forarm and hand.
Smith et al. J Hand Microsurg 2019; 11 (1): 1-5
Preoperative ultrasound in patients with meralgia paraesthetica to detect anatomical variations in the course of the lateral femoral cutaneous nerve.
De Ruiter et al. World Neurosurg 2021, epub ahead of print Feb 27
The LFCN shows variations in its course that might make it difficult to localize the nerve in surgery for meralgia paraesthetica. The authors reviewed 54 patients who underwent HRUS before surgery. As expected, there was a 100% correlation between ultrasound and intraoperative findings – strengthening what we believe: that US should be used as standard preoperative tool.
Ultrasound features of traumatic digital nerve injuries of the hand with surgical confirmation
Endo et al. Skeletal Radiol 2021; online ahead of print Feb 4
The authors describe findings in 29 injured digital nerves and which imaging plane was most useful for diagnosis of the 20 lacerations. Contrary to a first guess, they could document all injuries in short axis view, while it was more difficult or even not possible in long axis.
THE INTERESTING CASE
*Sonographic multifocal cranial nerve enlargement in multifocal acquired demyelinating sensory and motor neuropathy.
Oka et al. Intern Med 2021; epub ahead of print Mar 22
A young patient with MADSAM (a subtype of CIDP), who also had involvement of cranial nerves and exhibited focal swelling in the vagus and facial nerve. So don´t forget: with a HR-probe, you can also check out those! (especially the vagus is absolutely easy to find – see our Nerve Guide)
We wish you the best during these hard times. Stay safe.
Your Sonocampus Team
*This is a free article


Excellent
We say thank you for your nice comment.